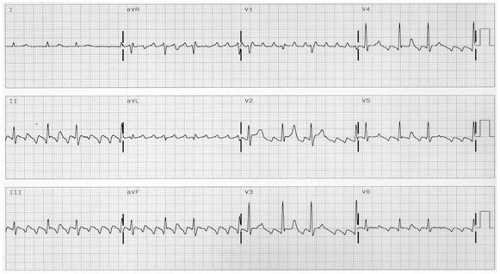
He was referred to the cardiac electrophysiology department for a typical atrial flutter ablation, which he underwent 2 weeks after initial presentation. In the absence of any new obstructive lesion, the reduced ejection fraction was thought to be due to tachycardia-induced cardiomyopathy, given the persistent atrial flutter and elevated ventricular rates. The patient presented to the cardiology department 5 days later for a coronary angiogram, which showed a patient bypass graft and severe native coronary artery disease. Ventricular rate control was achieved in a 74-year-old man after developing atrial flutter with exercise-induced 1:1 atrioventricular conduction 1 week earlier. The patient was discharged the next day at his own request. Ventricular rate control ( Figure 2) was achieved by titrating metoprolol tartrate to 100 mg twice daily, and the patient was given 20 m/g of rivaroxaban daily for stroke prevention. Because of the reduced ejection fraction and the history of known coronary artery disease, a coronary angiogram recommended. A transthoracic echocardiogram showed a mildly reduced ejection fraction of 40% to 45%. The cardiology department was then consulted for management. The treadmill test was urgently stopped, and after 2 minutes of recovery, symptoms resolved and 2:1 atrioventricular conduction resumed. One minute and 30 seconds into the treadmill test, a 1:1 atrioventricular conduction of the atrial flutter with a ventricular rate of 240 beats/min developed ( Figure 1). The patient underwent a myocardial perfusion exercise stress test the day after admission. 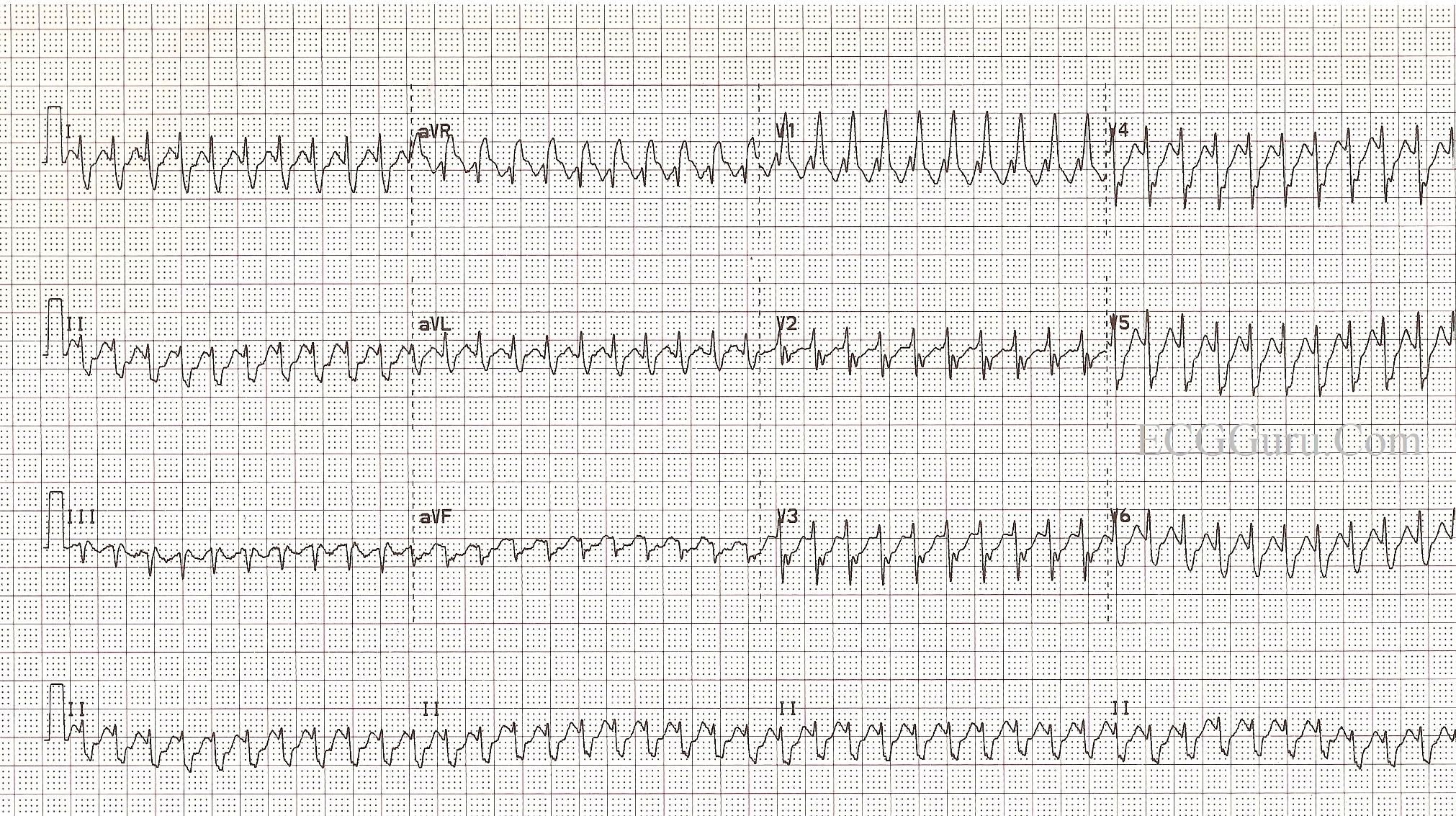 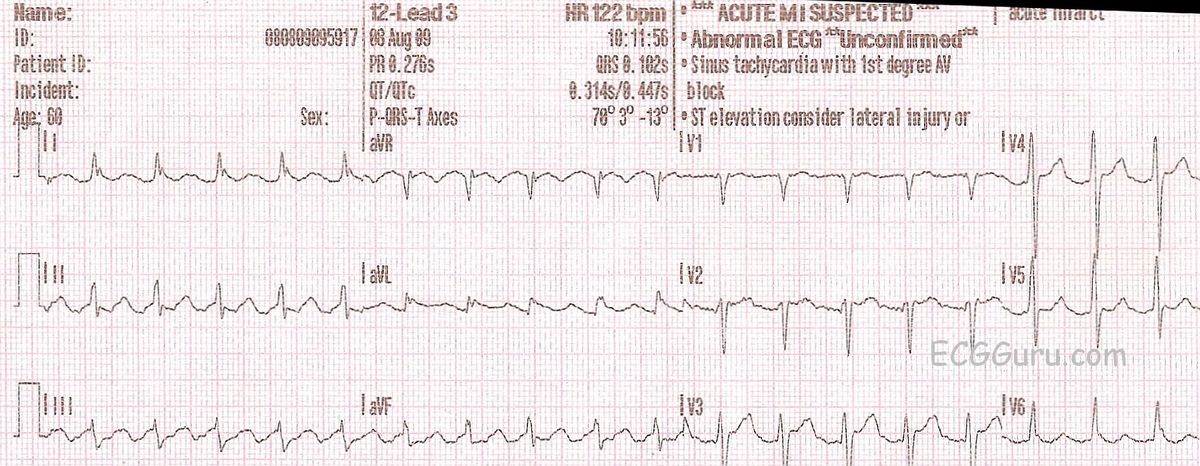
His current medications included metoprolol succinate, 25 mg/d lisinopril, 20 mg/d aspirin, 81 mg/d atorvastatin, 40 mg/d and metformin, 750 mg/d. His comorbidities included type 2 diabetes mellitus, obstructive sleep apnea, hypertension, and hyperlipidemia. He denied noticing any palpitations and also denied a history of syncope. His symptoms included sudden-onset dyspnea, lightheadedness, and chest tightness during peak exertion during the past year, which would resolve shortly after cessation of exercise. Report of CaseĪ 71-year-old man with a history of coronary artery disease and a 1-vessel coronary artery bypass graft 14 years earlier was admitted to the hospital with the diagnosis of typical atrial flutter with a rapid ventricular response (ventricular rate, 130 beats/min). 3 This report describes a case of atrial flutter with exercise-induced 1:1 atrioventricular conduction during an exercise stress test. 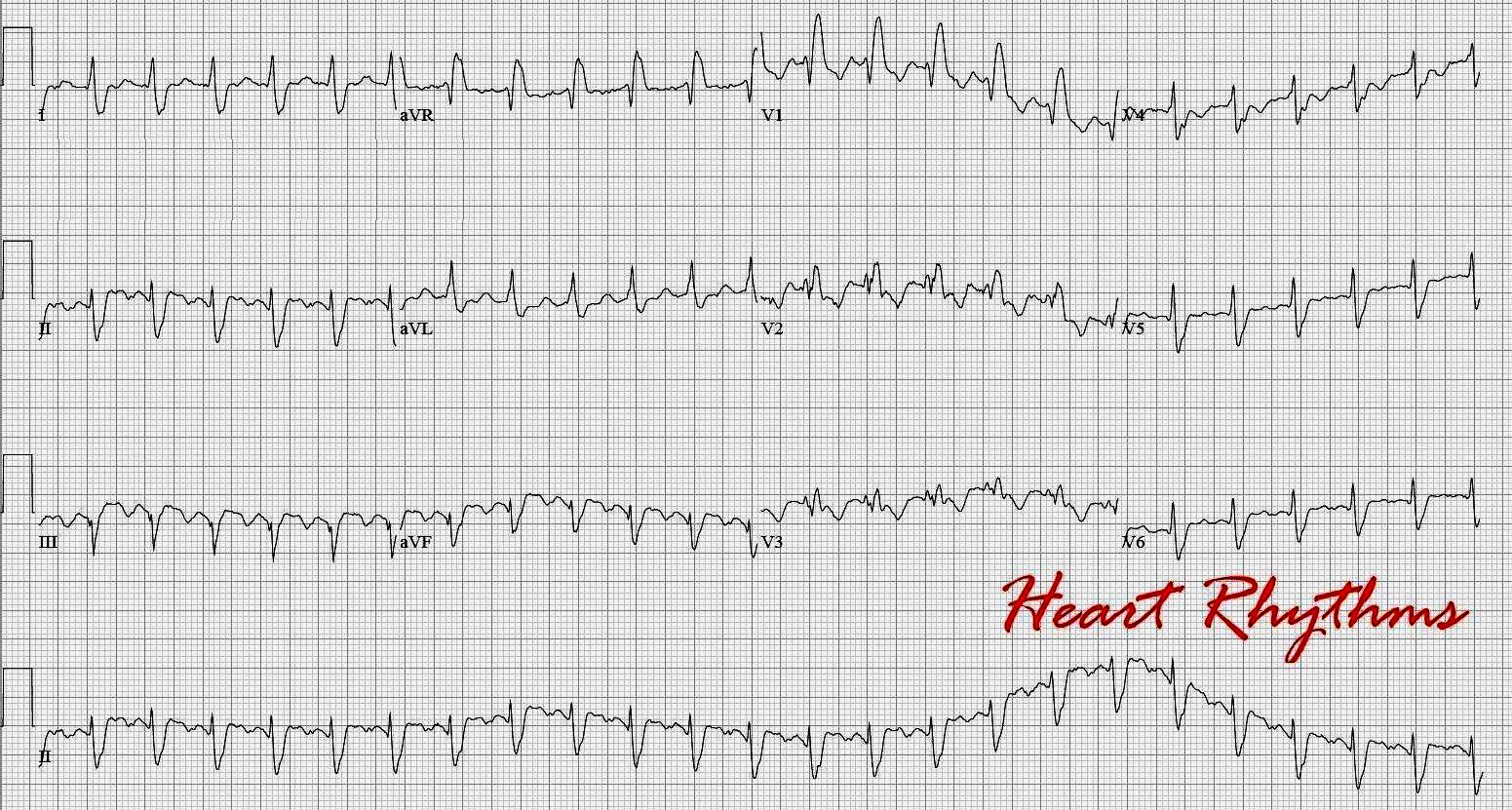
Atrial flutter with 1:1 atrioventricular conduction is a rare entity and has classically been described in the setting of class 1A or 1C antiarrhythmic drug therapy. Symptoms are often related to the rate of ventricular response and may include palpitations, dyspnea, chest pain, presyncope, or syncope. Atrial flutter often causes a ventricular rate of 150 beats/min in the absence of atrioventricular nodal blocking agents or atrioventricular nodal disease. 2 The ventricular rate usually occurs in multiples of the underlying atrial fibrillation rate (eg, 2:1, 3:1, 4:1), as the physiologic properties of the atrioventricular node limit the number of impulses that can reach the His-Purkinje system. 1 Atrial flutter typically results in an atrial rate of 250 beats/min to 350 beats/min. 1 Risk factors for developing atrial flutter include hypertension, heart failure, valvular disease, acute and chronic lung disease, alcohol use, and metabolic disturbances. 1 The incidence of typical atrial flutter increases with age, comorbidities, and any disease process that results in secondary atrial dilation. Atrial flutter is a commonly encountered arrhythmia in clinical practice, with an estimated incidence of 88 per 100,000 person-years.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
